This article explains the WiscMed team’s thoughts on pneumatic otoscopy in primary care and why we choose not to implement this capability in the Wispr.
The purpose of pneumatic otoscopy is to determine the mobility of the tympanic membrane (eardrum). Evaluating mobility may be useful when considering diagnoses of acute otitis media (AOM), otitis media with effusion (OME), eustachian tube dysfunction and eardrum perforation. Performing pneumatic otoscopy requires significant clinical skill; the clinician must obtain a tight seal between the otoscope and the external ear canal while simultaneously squeezing an air bulb and watching the tympanic membrane for movement.
Some experienced providers feel strongly that pneumatic otoscopy is central to the correct diagnosis of Acute Otitis Media (AOM). However, UpToDate information on diagnosis of AOM includes the following observations:
- Pneumatic otoscopy can be painful in children with AOM. It is not necessary in children with bulging tympanic membranes because all bulging tympanic membranes have decreased or absent mobility.
- A bulging tympanic membrane is the hallmark of AOM and differentiates AOM from otitis media with effusion (OME). A bulging tympanic membrane indicates both acute inflammation and middle ear effusion (MEE, and thus decreased or absent mobility).
- Decreased or absent mobility cannot be used in isolation to make a diagnosis of AOM because it does not distinguish infected from uninfected middle ear fluid. In a study correlating examination findings with a diagnosis of AOM by experienced otoscopists, decreased mobility of the tympanic membrane was present in all 50 cases of AOM and 23 of 34 cases of OME.
- The diagnosis of MEE can be made by the presence of physical findings including opacification of the TM or visible air fluid levels. Thus OME can be reliably determined in the non-bulging TM with either of these physical findings.
UpToDate makes the following additional points.
A clinical diagnosis of AOM can be made in children with either [1,2]:
- Bulging of the tympanic membrane; distinct fullness or bulging of the tympanic membrane is the most specific and reproducible sign of acute inflammation. Pneumatic otoscopy is not necessary in children with bulging of the tympanic membrane.
- Perforation of the tympanic membrane with acute purulent otorrhea if acute otitis externa has been excluded.
In addition to the above UpToDate points, it is becoming rare for physicians outside of a select group of highly-trained pediatricians and otolaryngologists to be facile with the skill and coordination required to perform pneumatic otoscopy. In the right hands, pneumatic otoscopy may play a role in the evaluation of the acute ear by specialists, but it is secondary to good visualization by the primary care physician.
The American Academy of Pediatrics (AAP) makes the following recommendations in their 2013 “The Diagnosis and Management of Acute Otitis Media [2]:”
- Key Action Statement 1A: Clinicians should diagnose acute otitis media (AOM) in children who present with moderate to severe bulging of the tympanic membrane (TM) or new onset of otorrhea not due to acute otitis externa. Evidence Quality: Grade B. Strength: Recommendation.
- Key Action Statement 1B: Clinicians should diagnose AOM in children who present with mild bulging of the TM and recent (less than 48 hours) onset of ear pain (holding, tugging, rubbing of the ear in a nonverbal child) or intense erythema of the TM. Evidence Quality: Grade C. Strength: Recommendation.
Our goal with the Wispr otoscope is to give the front-line clinician the best chance of seeing the eardrum. To increase the likelihood of success in seeing the eardrum, the speculum must be as small as possible, and the camera must be at the far end of the speculum. With proper visualization, bulging and perforations are clearly seen and the need for pneumatic otoscopy is diminished.
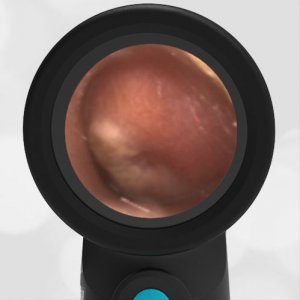
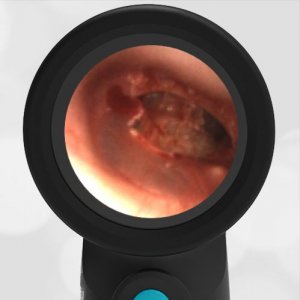
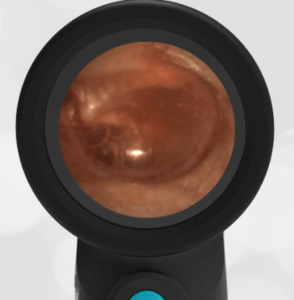
These are examples illustrating the power of the WiscMed Wispr digital otoscope to diagnose common conditions without the use of pneumatic otoscopy.
- Acute Otitis Media
- Blast Injury
- Otitis Media with Effusion
- Normal Ear
In a cooperative patient, the Valsalva maneuver can be used to evaluate eardrum mobility.
If a digital otoscope with pneumatic otoscopy is important to your practice, here is a review article of digital otoscopes researched and authored by WiscMed. Several of the digital otoscopes reviewed support pneumatic otoscopy.
References
- Shaikh N, Hoberman A, Rockette HE, Kurs-Lasky M. Development of an algorithm for the diagnosis of otitis media. Acad Pediatr 2012; 12:214.
- Lieberthal AS, Carroll AE, Chonmaitree T, et al. The diagnosis and management of acute otitis media. Pediatrics 2013; 131:e964.