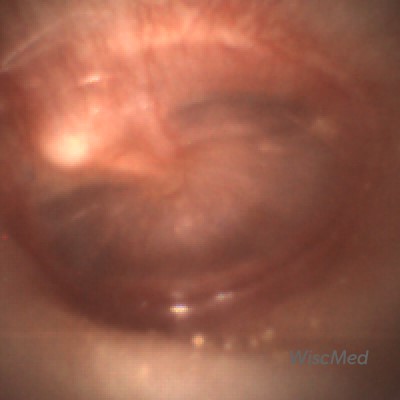
Acute Otitis Media (AOM) – a spectrum of images from normal to AOM
A challenging problem during an ear exam is differentiating between a 1) normal ear, 2) a “red ear,” 3) middle ear effusion (MEE) and 4) acute otitis media (AOM).
There are two aspects to this challenge. The first is obtaining a diagnostic view of the tympanic membrane. The second is knowing the features of the tympanic membrane that differentiate the possible diagnoses.
Obtaining a diagnostic view of the tympanic membrane (ear drum)
Obtaining a diagnostic view of the tympanic membrane (TM) has been a challenge, especially in the pediatric population. The challenge is due to three reasons;
1. The pediatric ear canal is small; about half the diameter of an adult canal
2. The pediatric ear canal is usually at least partially occluded by ear wax (cerumen)
3. The pediatric patient often does not hold still for the exam
Traditional analog otoscopes found in every clinic room rely on a light, a funnel and a magnifying glass. The practitioner is required to place their eye close to the magnifying glass and attempt to see down the funnel to the ear drum. Often this visual pathway is obstructed by cerumen. In the case of cerumen obstruction, an attempt must be made to remove the cerumen using a curette. Contact between the curette and the ear canal is uncomfortable. It is technically challenging to perform this procedure in the narrow confines of the ear canal, with limited visualization of the working area.
The Wispr digital otoscope by WiscMed solves the challenge of obtaining a diagnostic view of the tympanic membrane. The Wispr incorporates a nano camera at the very end of the speculum. The speculum is small enough that it can navigate through a small window in the cerumen. A full-field view of the tympanic membrane, past any cerumen, is possible. In addition, using video mode allows for the exam to be recorded. Using video, the practitioner can focus on the exam, knowing that even a brief glimpse of the tympanic membrane that might not be mentally processed in real time can be reviewed at leisure from the video after the exam.
Once the entire view of the tympanic membrane is obtained, a proper diagnosis can be obtained.
Making the Diagnosis
1) A normal ear has a number of clear features. The tympanic membrane is often described as “pearly grey.” The ear drum in convex inwards. The malleus bone is clearly visible. Often, the incus bone is visible. The deeper stapes bone and the chorda tympani nerve are sometimes visible.
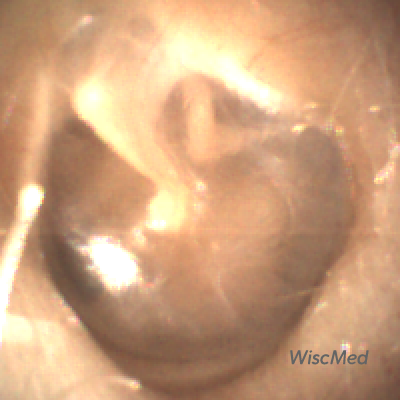
Normal left ear without annotations

Normal left tympanic membrane showing all three bones of the middle ear
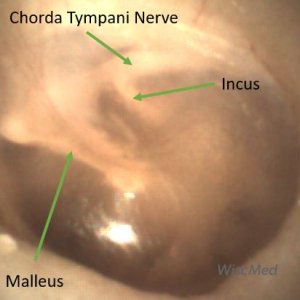
Normal left tympanic membrane showing the chorda tympani nerve
2) An erythematous (red) ear has all of the features of the normal ear. The distinction in this case is that the tympanic membrane may appear slightly red, or the vasculature on the malleus may be prominent. The tympanic membrane in this case is not bulging, and there are no fluid levels present behind the ear drum. Causes of an erythematous ear include crying, mild trauma, dehydration, fever, recent body position (supine vs upright), elevated blood pressure and medications that dilate vasculature. A red ear alone does not signify infection and antibiotics are not indicated.
- Prominent vasculature on the malleus
- Erythematous tympanic membrane
3) Middle ear effusion (MEE) of an ear will generally appear erythematous (red) and in addition will have air fluid levels visible behind the TM. The fluid levels are secondary to inflammation, generally from an infection of a viral nature. The presence of the air in the fluid suggests that the eustachian tube that drains to the nasal cavity is functioning correctly. A middle ear effusion indicates inflammation, but is not an indication for antibiotics.

Middle ear effusion (MEE) of the left ear

Another example of MEE of the left ear
4) Acute otitis media (AOM) appears as an “angry doughnut.” There is loss of all the normal landmarks of the tympanic membrane. The tympanic membrane is bulging outward and is generally erythematous with pronounced vasculature. The bulging of the tympanic membrane is from fluid in the middle ear space that is not draining due to the eustachian tube blockage. The pressure in the middle ear space can be uncomfortable. Treatment is focused on NSAID analgesia and antibiotics will often be administered. Here is an article reviewing the development and resolution of acute otitis media.
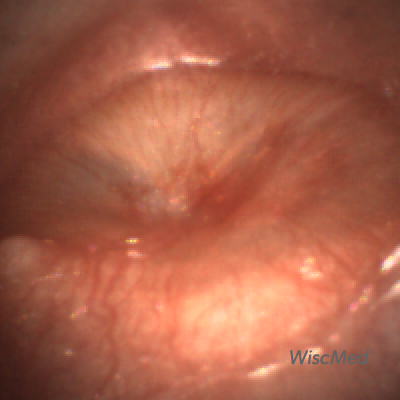
Acute Otitis Media (AOM)
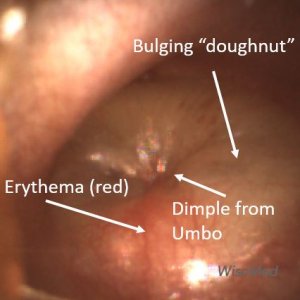
Acute Otitis Media (AOM) features

Acute otitis media (AOM)
James Berbee MD
Emergency Physician
Founder, WiscMed