Hemotympanum
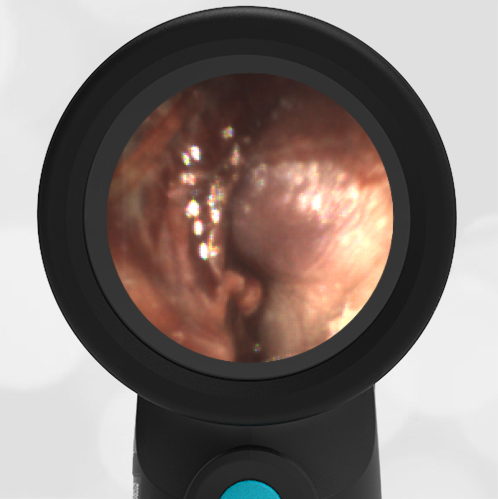
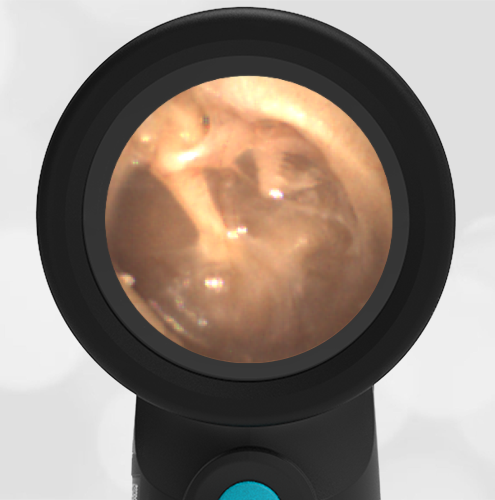
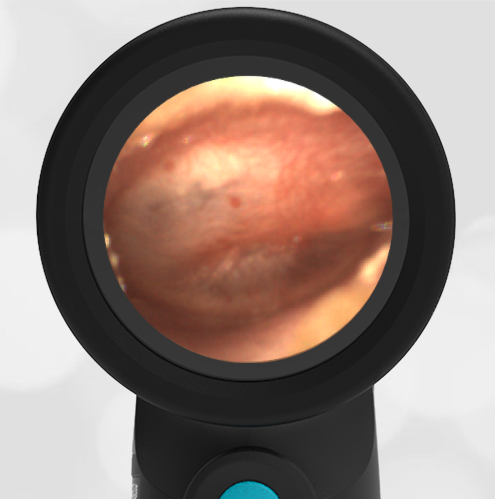
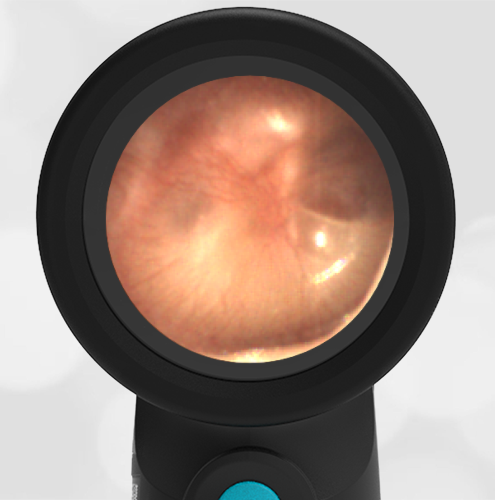
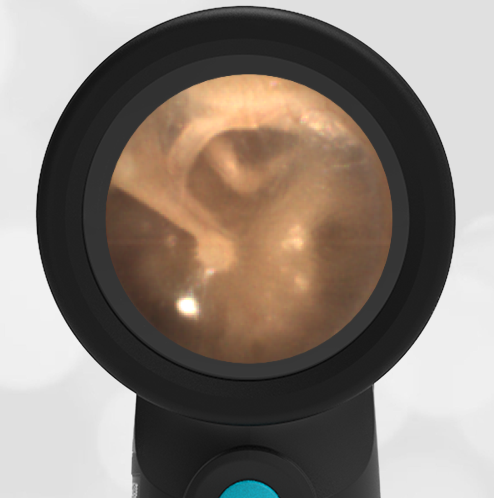
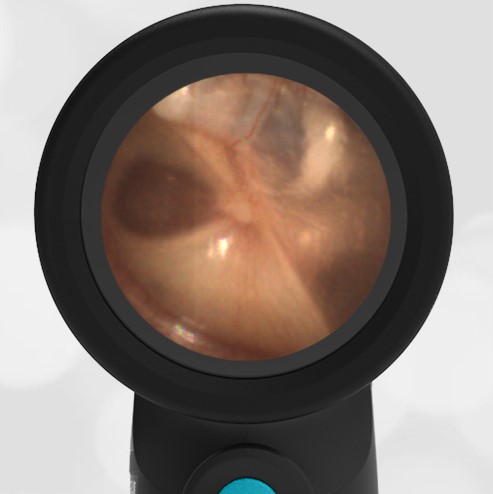
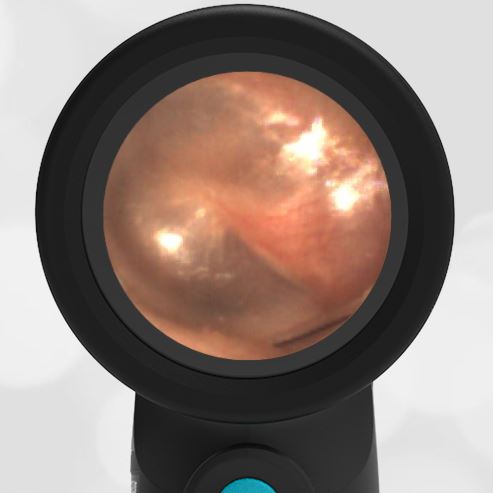
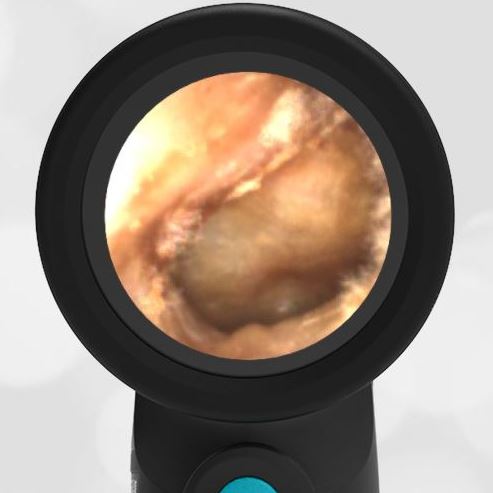
A previously healthy 3 year-old female presented to the ED for head injury. The child was being carried by her father when he accidentally tripped and fell forward. The back of the child’s head struck the cement sidewalk—reportedly quite forcefully. However, there was no LOC, altered mental status, or vomiting. The child complained of a headache but otherwise had no other symptoms. The parents felt that “she appeared normal” to them but brought her in for evaluation because of the headache. On examination the child was smiling, interactive and had no swelling, step-offs, or other deformities to her head. She had an entirely normal neurologic examination. Wispr examination revealed this image.
This child’s Wispr examination demonstrates a darkened, bulging TM consistent with hemotympanum (blood behind the ear drum).
In the setting of head trauma, hemotympanum typically occurs as a result of a basilar (lower) skull fracture with subsequent bleeding into the middle ear space.
Hemotympanum is often the earliest sign of basilar injury. Other later physical exam findings may include “raccoon eyes,” and bruising behind the ear. Despite the child’s well-appearance (she was deemed PECARN negative), the finding of hemotympanum led the clinicians to pursue neuro-imaging that revealed a minimally displaced temporal bone fracture. The patient was admitted to the pediatric neurosurgery service for observation and recovered uneventfully from her injury without intervention.
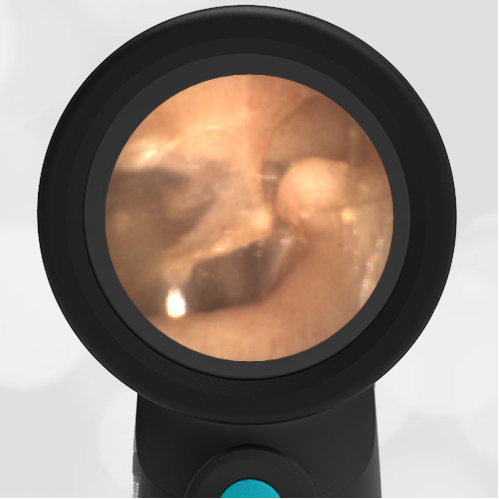
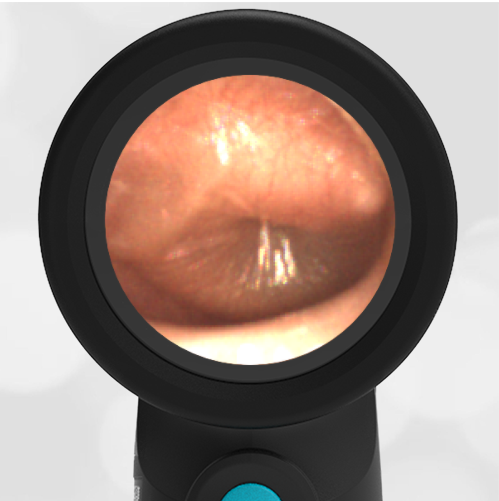
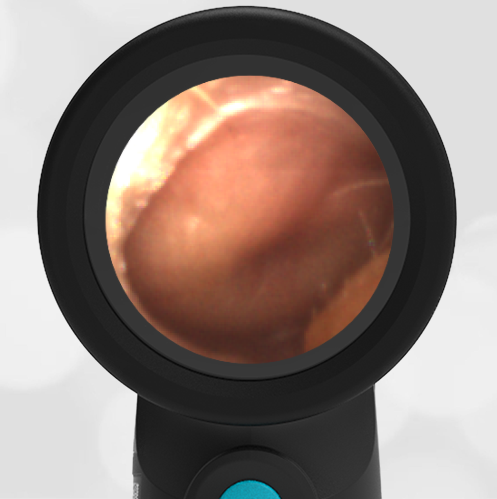
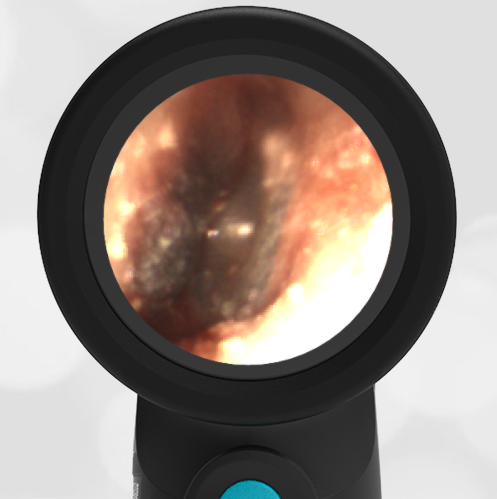
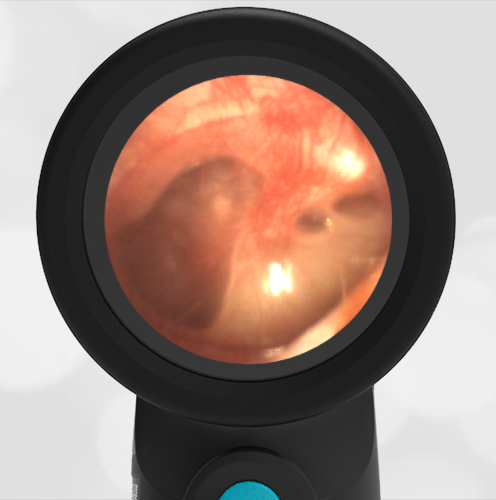
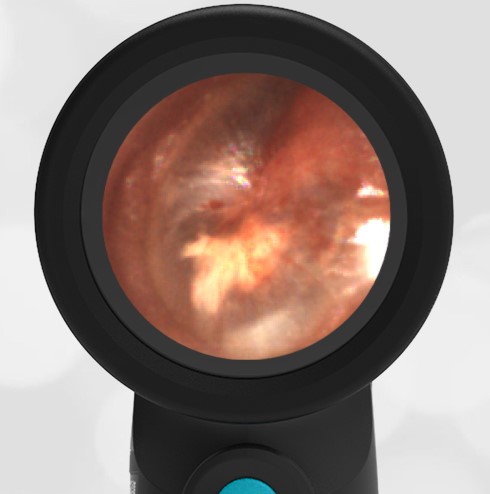
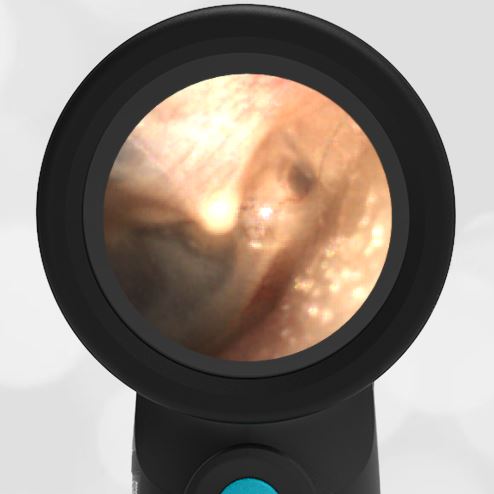
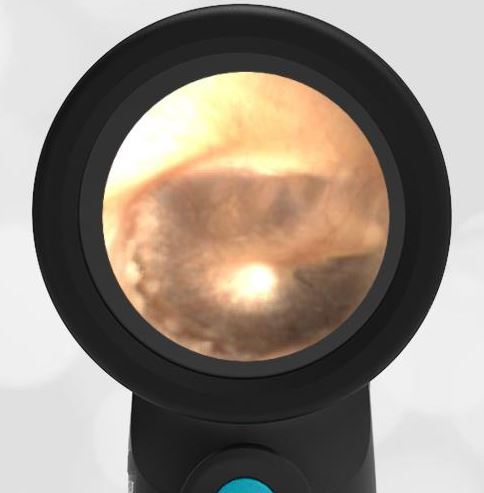
Interestingly, in this case, the initial evaluation was performed by standard otoscopy and reported as “a little dark in the canal, but otherwise normal”—a fact that demonstrates the challenge of viewing a non-perforated hemotympanum with a traditional otoscope. Light does not reflect strongly off the darkened TM which, combined with small canal diameter and the brief view so common in pediatrics, results in an incomplete assessment of the TM. Furthermore, just as with otitis media, not all hemotympanum appear the same (see the image below from a 10-year-old child who fell from a barn loft and sustained a complicated basilar skull fracture). In both cases, the WiscMed Wispr achieved diagnostic images that assisted clinicians with the correct neurologic workup, diagnosis, and treatment.

Hemotympanum in a 10 year old
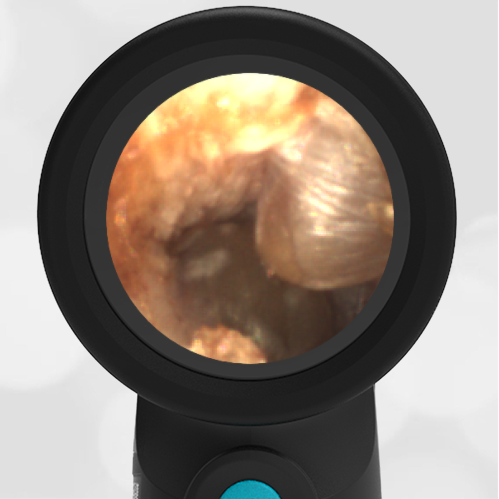
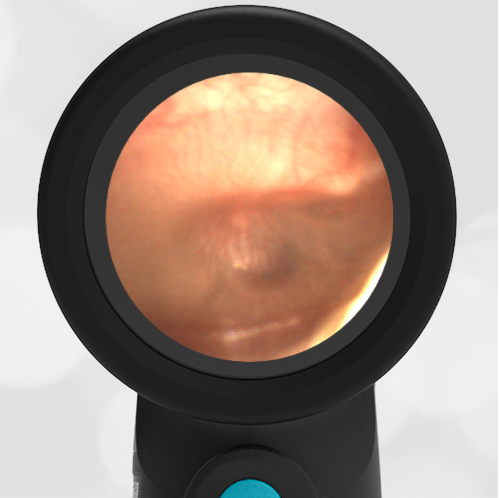
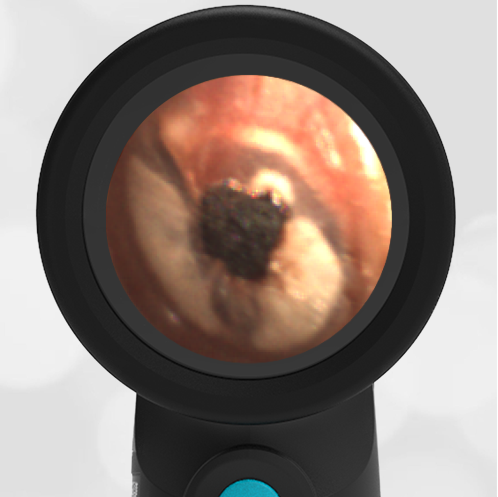
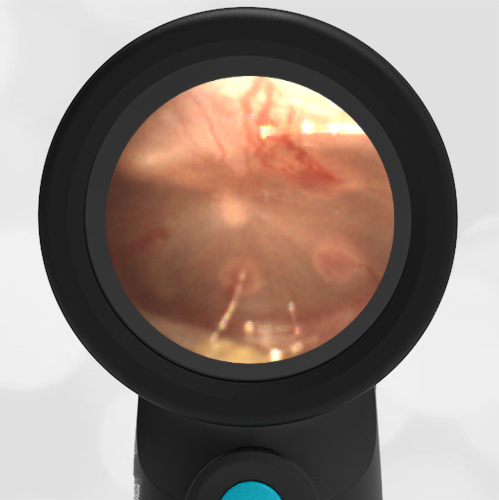
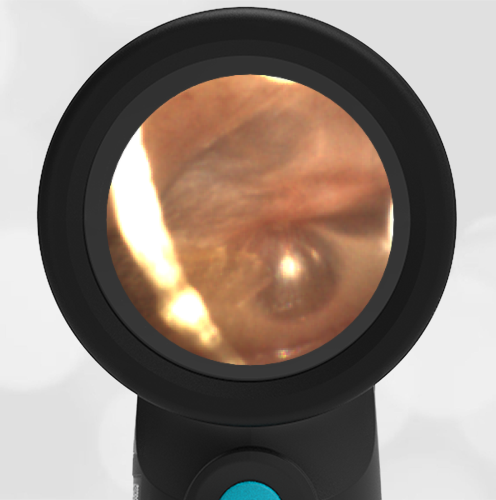
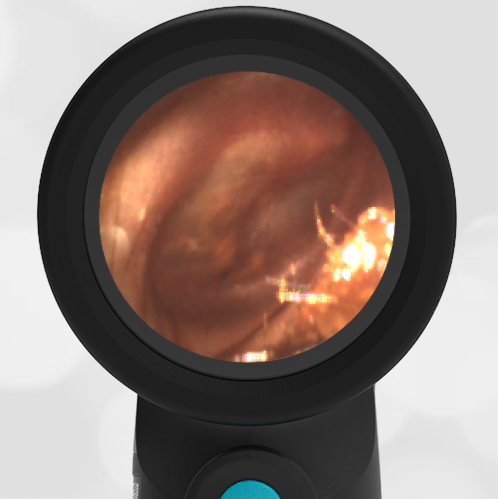
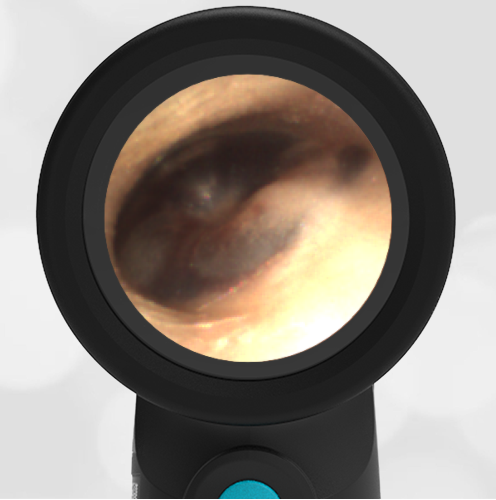
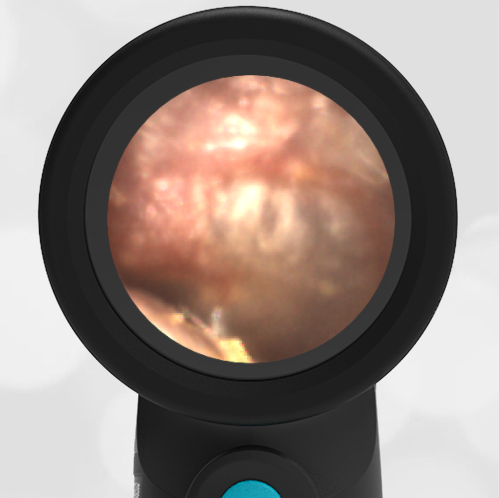
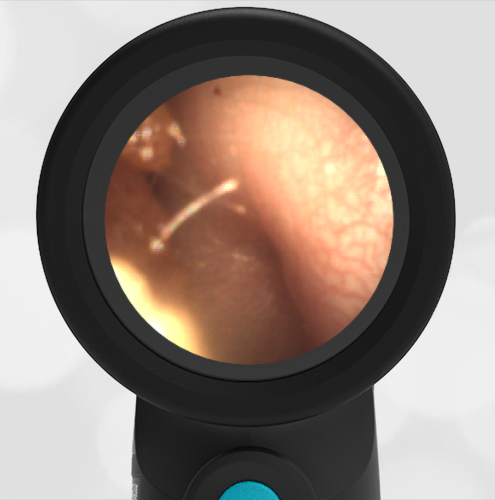
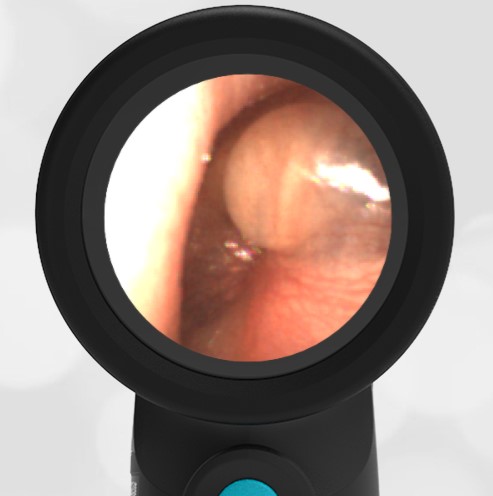
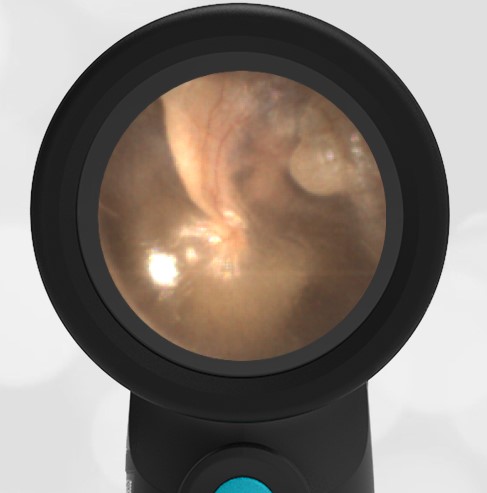
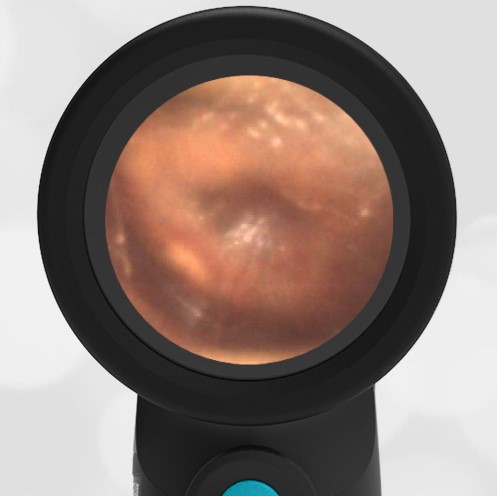
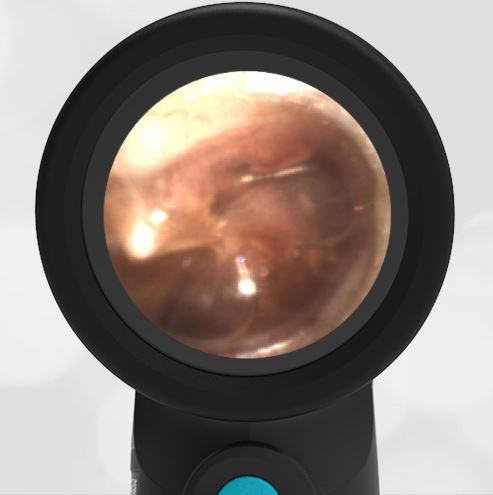
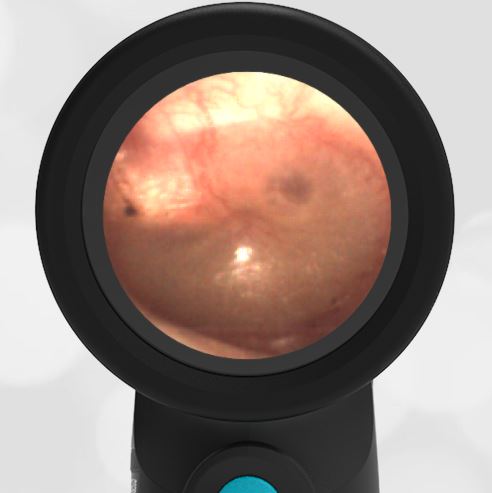
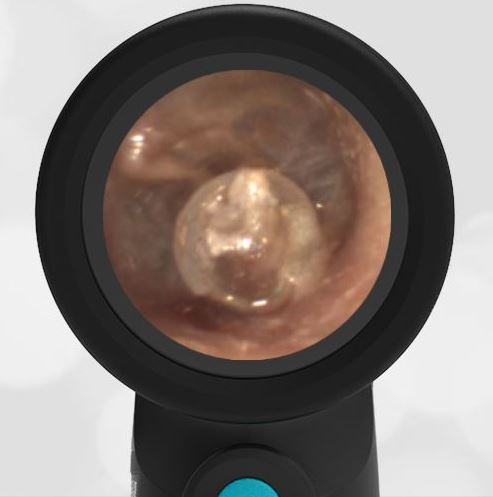
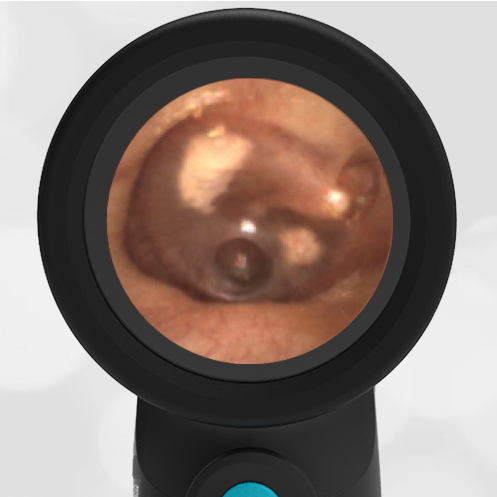
Here is another case that shows bilateral hemotympanum caused by epistaxis (nose bleed).