Perforation – June 6, 2024
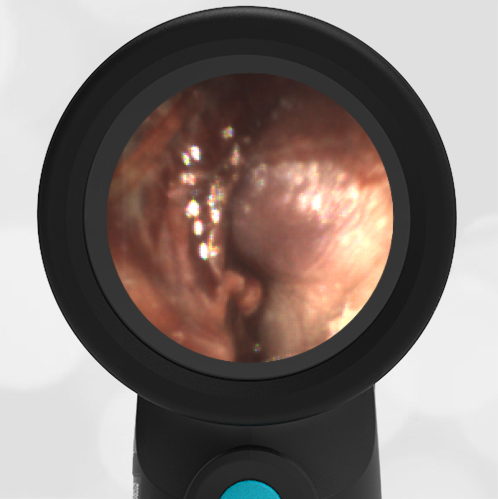
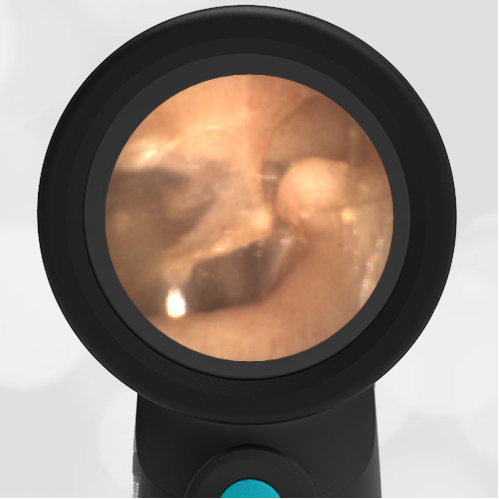
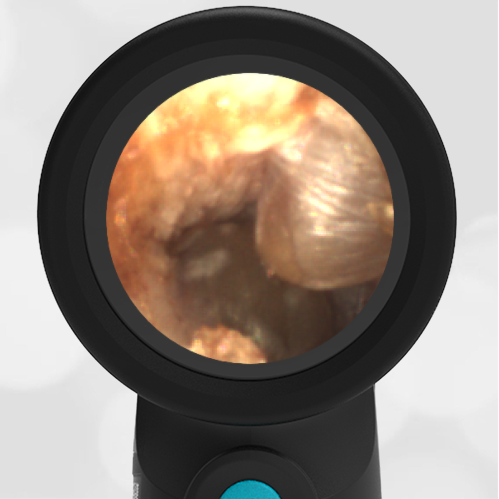
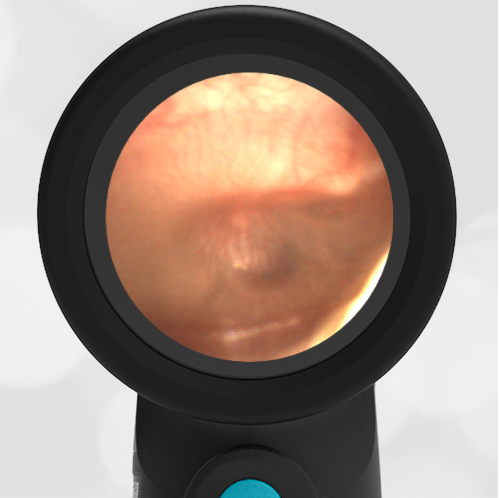
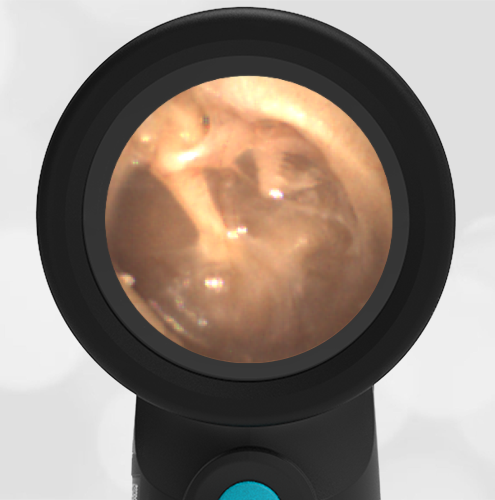
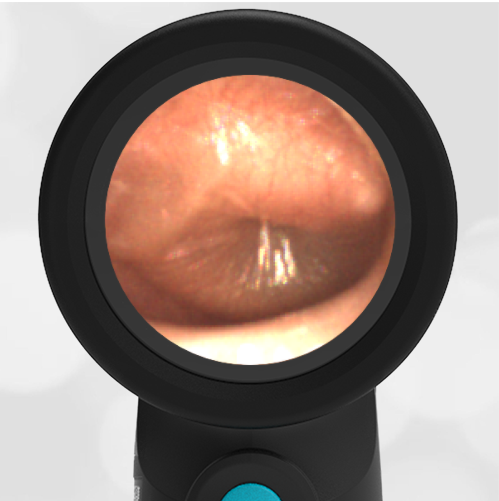
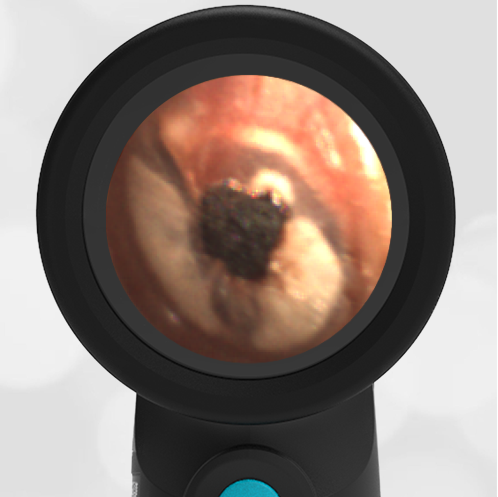
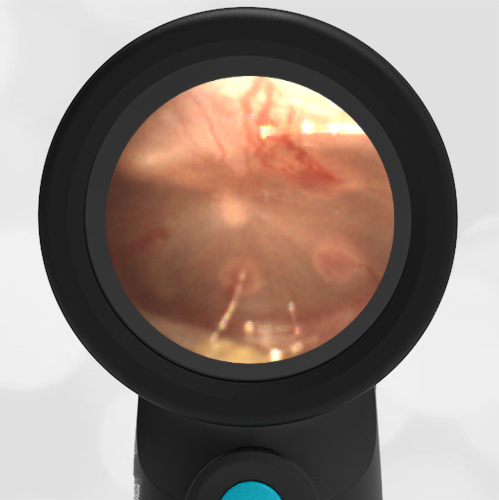
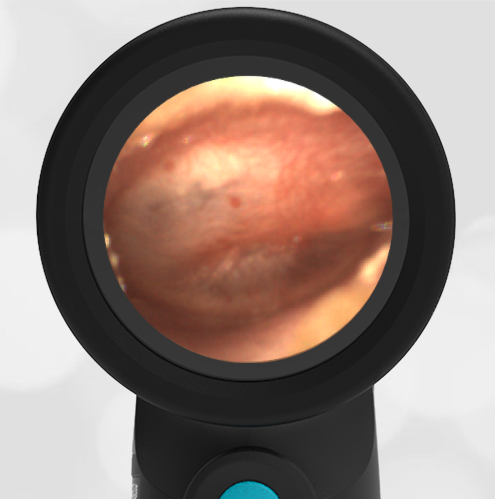
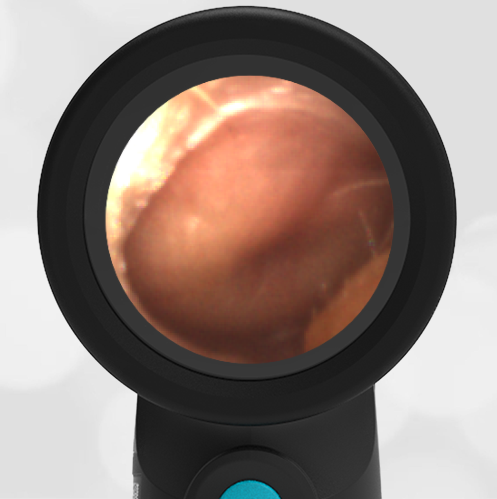
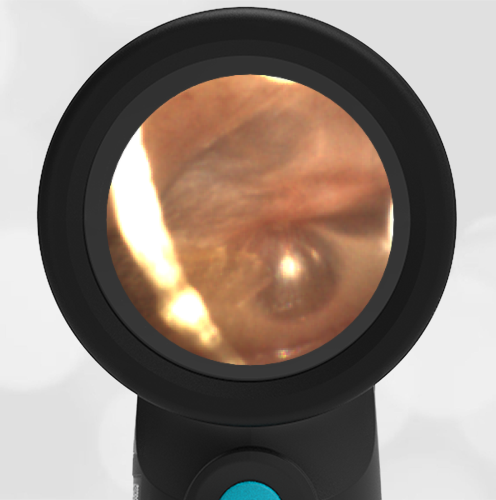
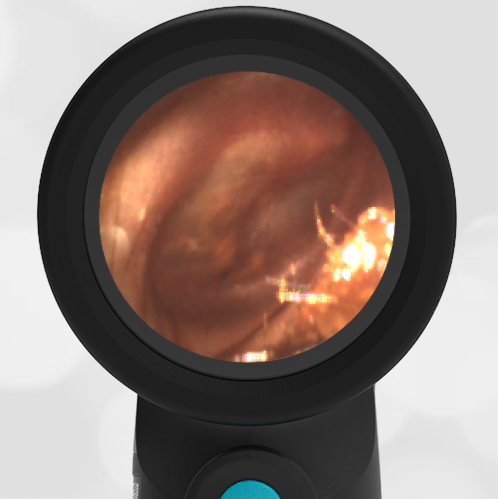
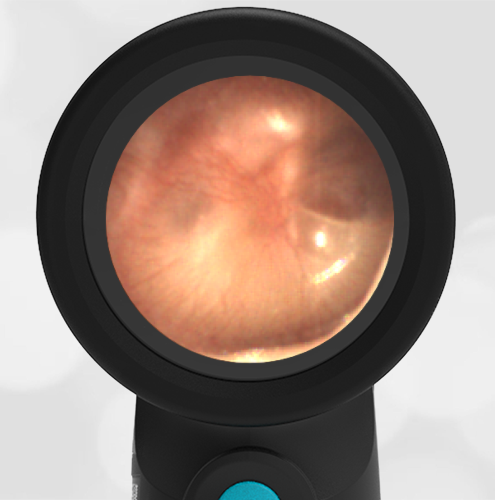
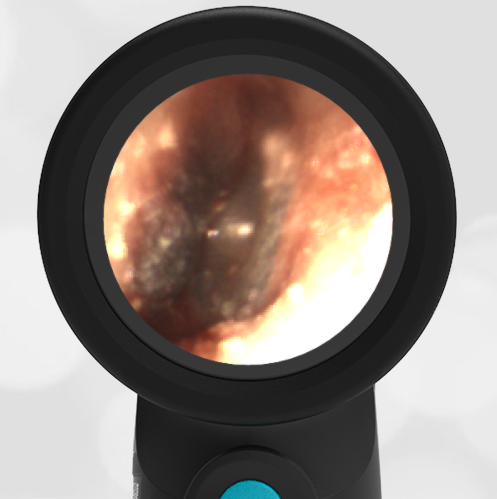
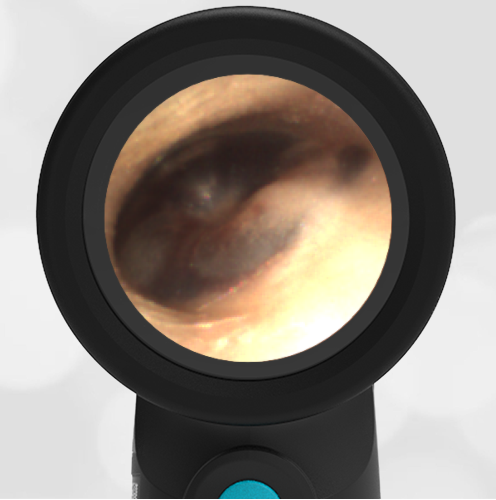
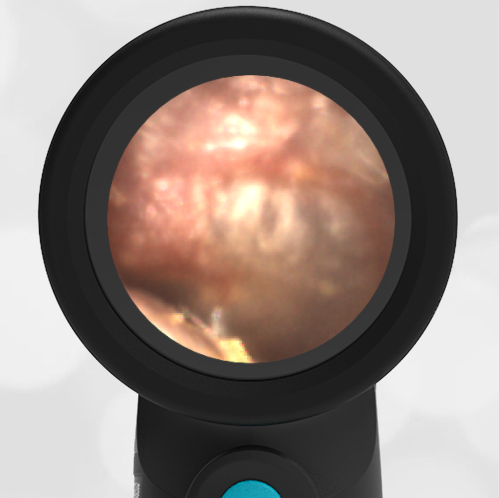
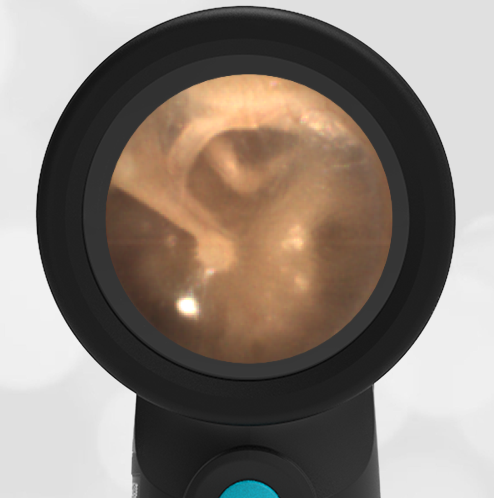
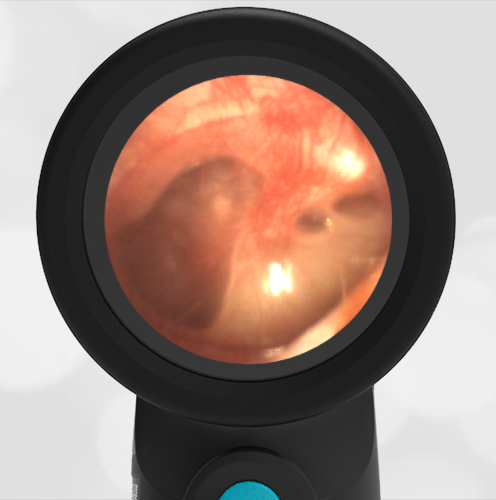
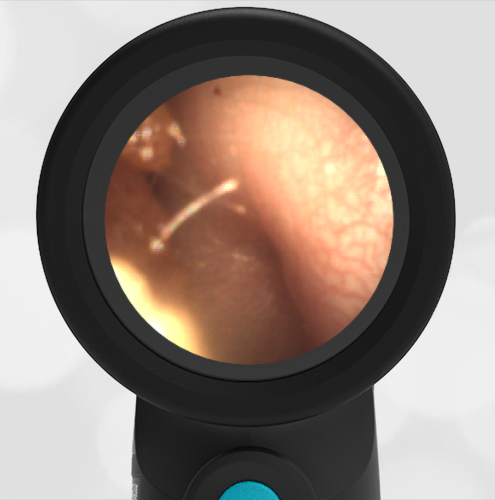
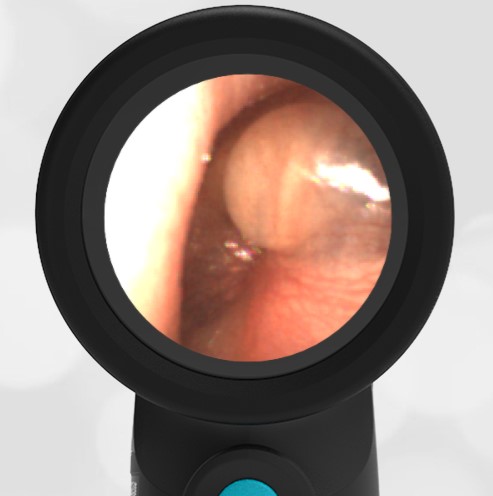
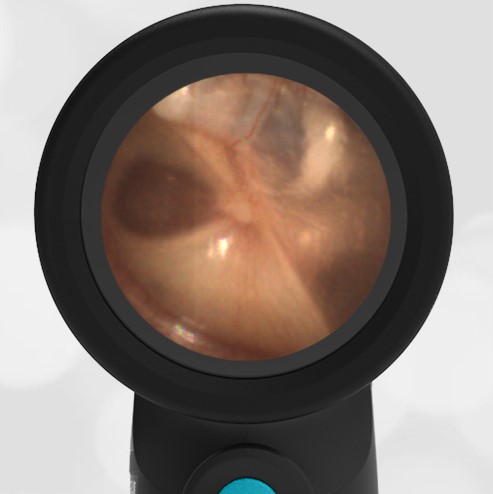
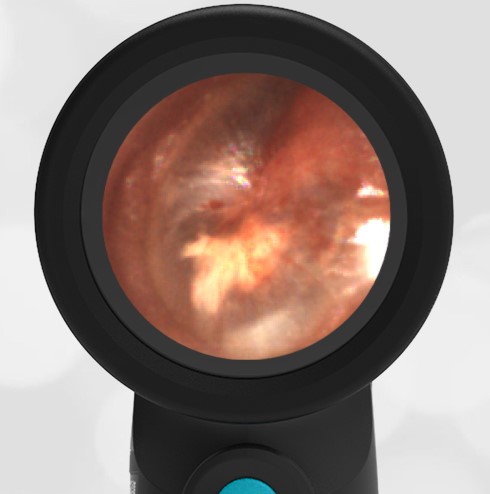
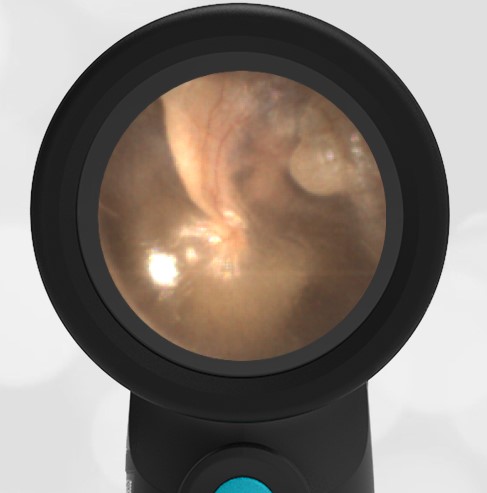
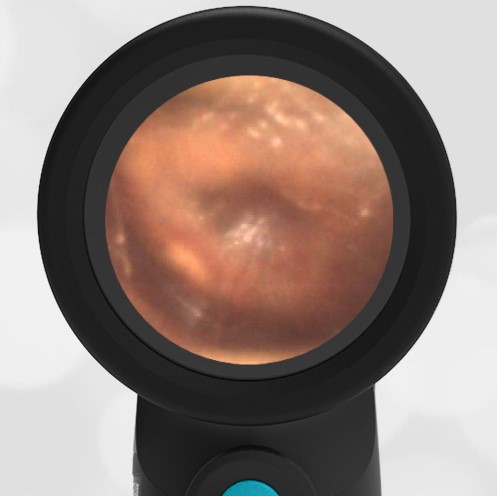
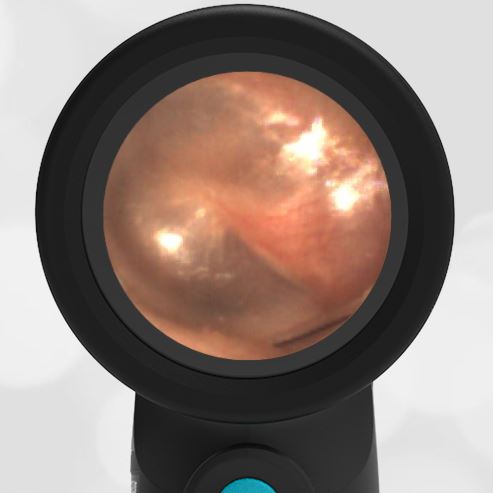
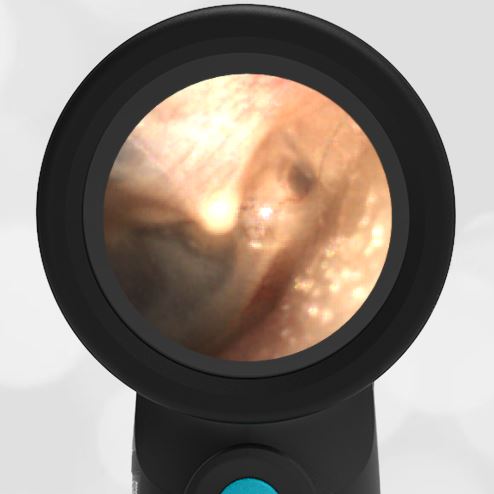
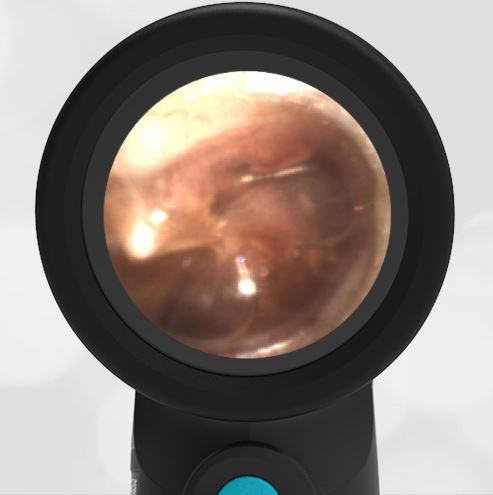
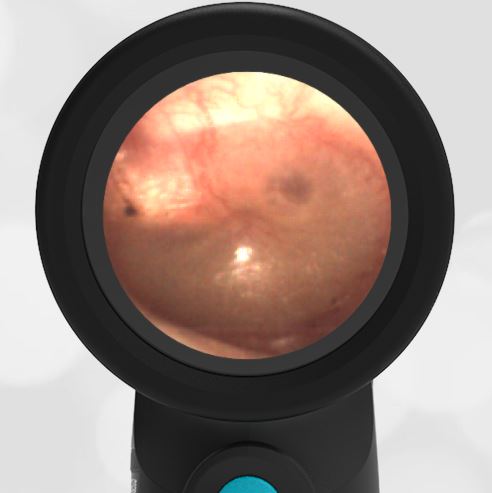
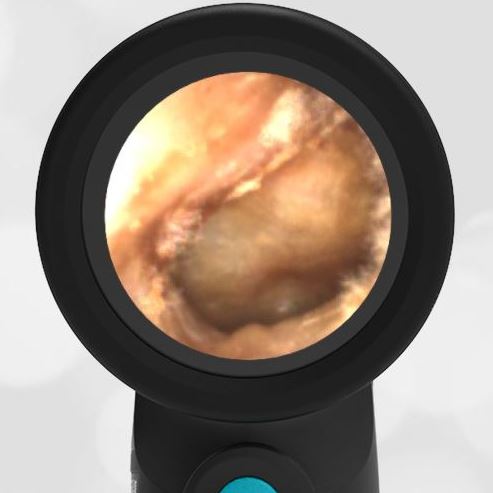
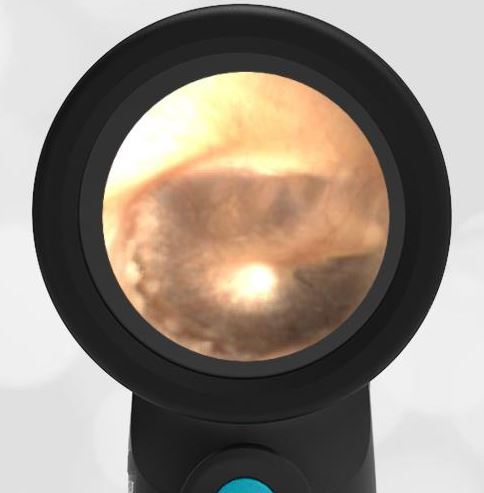
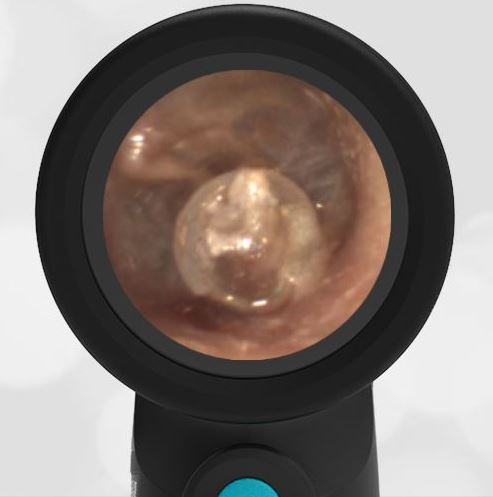
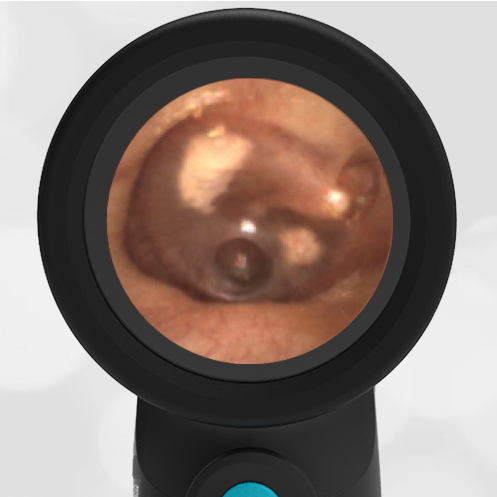
A 16-month-old presents to the emergency department (ED) with congestion and fever for one day. Her mom is worried she may have an ear infection due to past ear complaints, including a procedure performed on her left ear 5 months ago. Mom reports this surgery was necessary after her daughter had ear drainage and a diagnosis of ruptured left eardrum when she was only 4 weeks old. The child recovered uneventfully, and the current complaint is her first febrile illness since the surgery. In the ED, she is well-appearing and has mild upper respiratory (URI) symptoms. Her Wispr digital otoscopic exam is shown.
Which of the following does her Wispr exam demonstrate?
- Cholesteatoma
- Tympanic perforation
- Myringosclerosis
- Acute otitis media (AOM)
- B & C
Answer: E. Both tympanic perforation and myringosclerosis.
The child’s Wispr exam demonstrates both myringosclerosis (anterior superior) and a tympanic membrane (TM) perforation (posterior inferior). There is no drainage or bulging to indicate acute otitis media (AOM). Upon further review of the child’s medical records, the procedure performed on her left TM was a resection of a congenital cholesteatoma and gelfoam tympanoplasty. The gelfoam has been extruded/absorbed and she has a resultant perforation that is closely monitored.
A cholesteatoma is an epithelial-lined cyst of the TM that may invade the middle ear space and impact hearing. Congenital cholesteatomas appear as small pearly bumps, typically on the anterior portion of the TM (image). While felt to be relatively rare, the incidence of congenital cholesteatomas is likely underestimated with one review estimating as high as 24%. In the current case, the unusual drainage and concern for AOM in the neonatal period led to an appropriate referral to the Pediatric ENT specialist.
On this visit, no action is required.
Here is the complete video of the exam.
Reference: