Hemotympanum
A 3-year-old child is brought to a rural emergency department for evaluation of injury after being dropped by a “tall” family member, landing on his face. He cried immediately and seemed to be acting normally, however his parents became worried when he developed swelling and bruising over his right eye. He reportedly had no other findings to suggest additional injury. Given the eye bruising and mechanism, a CT of his head was performed that demonstrated a fracture through the superior orbital roof. The child was transferred to a pediatric trauma center for further evaluation where his Wispr examination revealed this image.
What is your diagnosis?
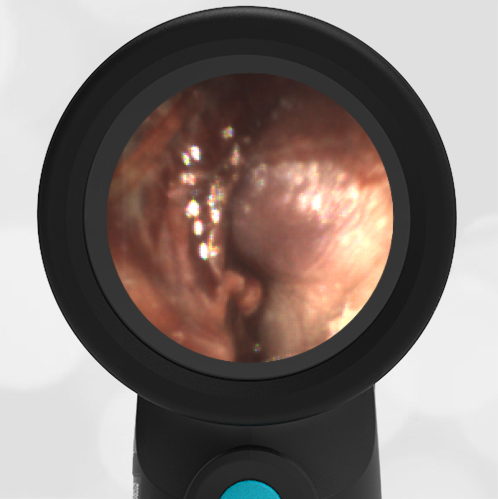
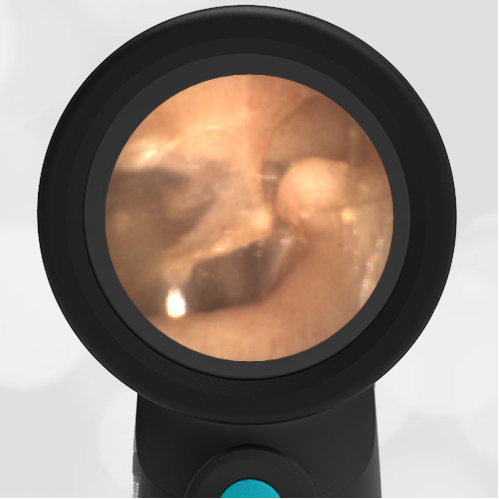
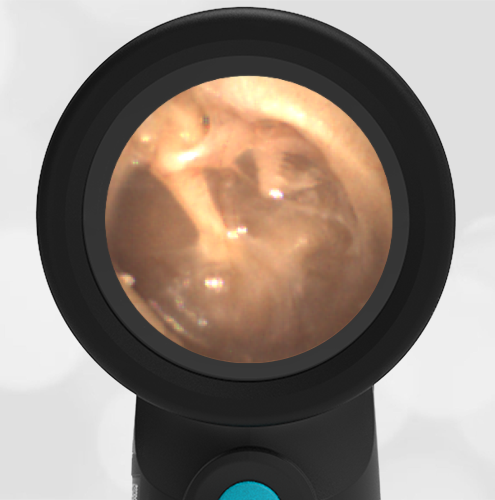
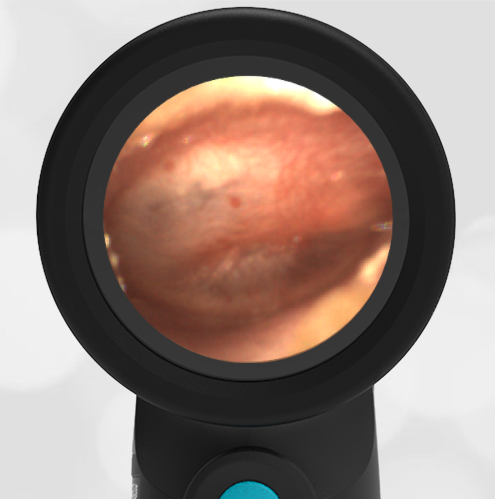
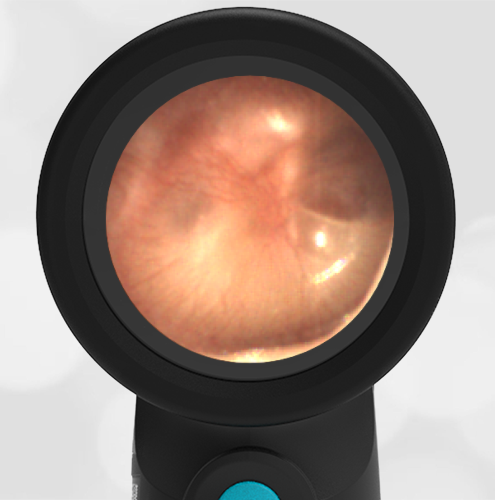
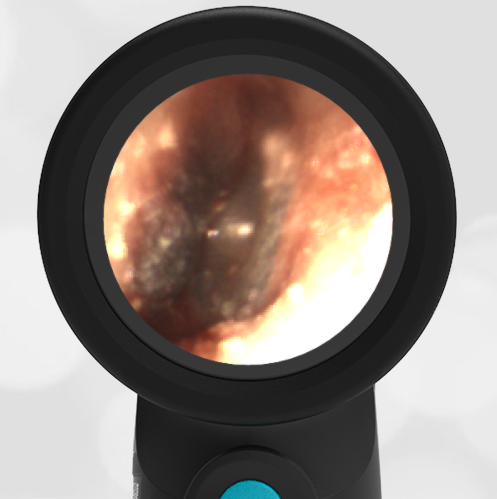
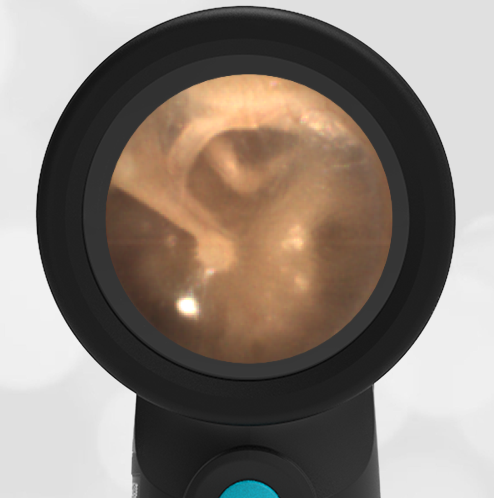
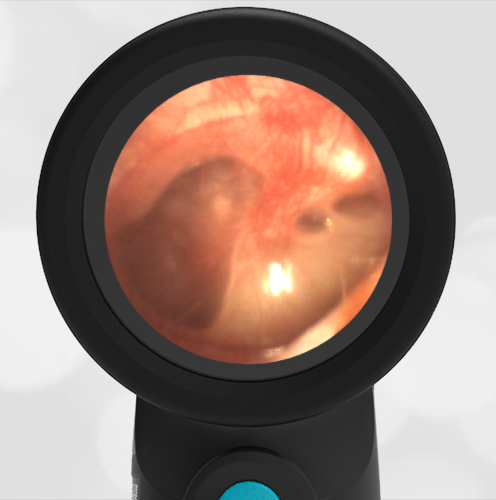
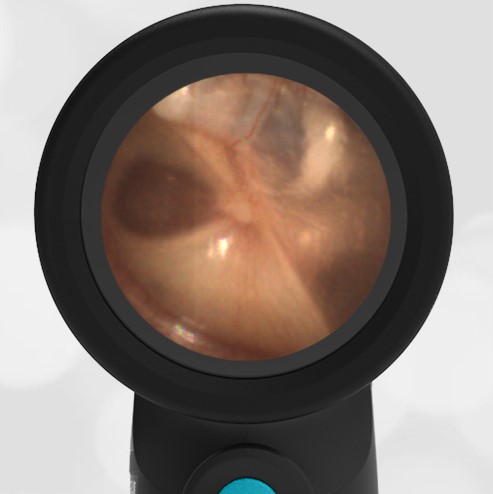
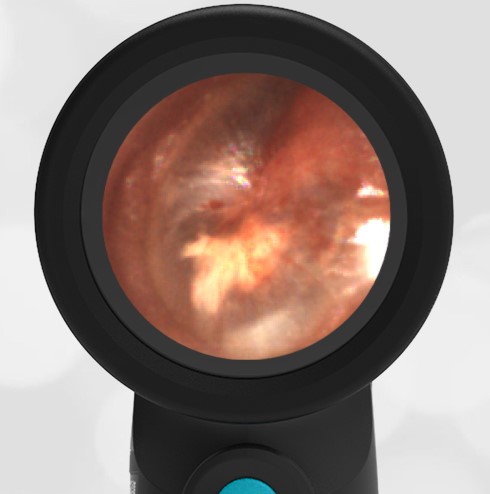
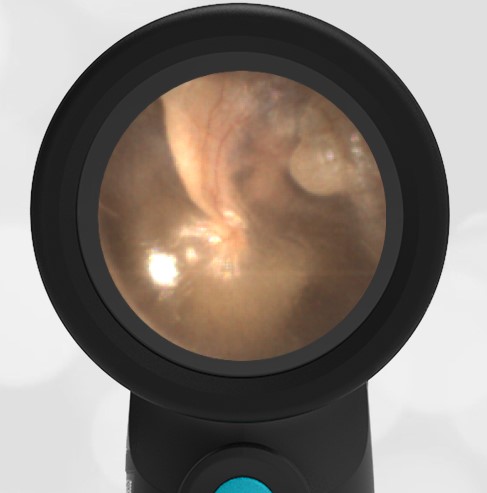
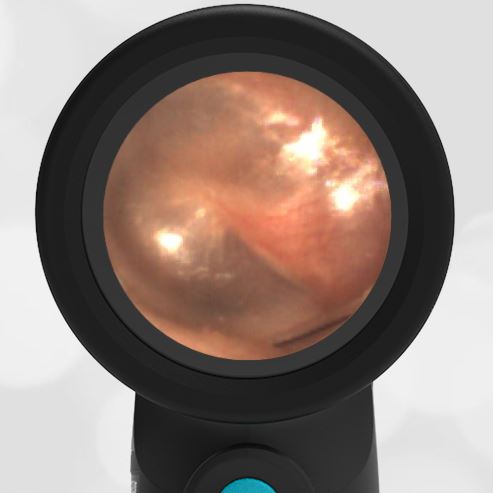
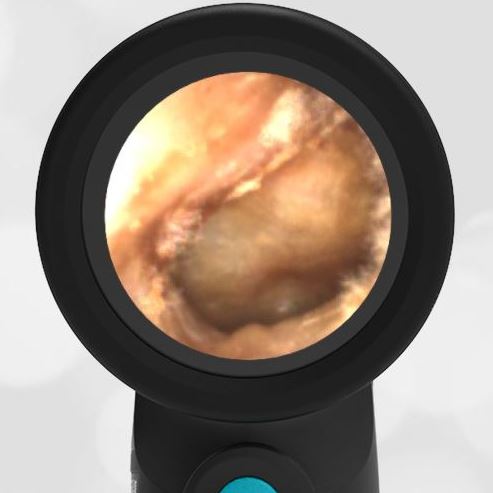
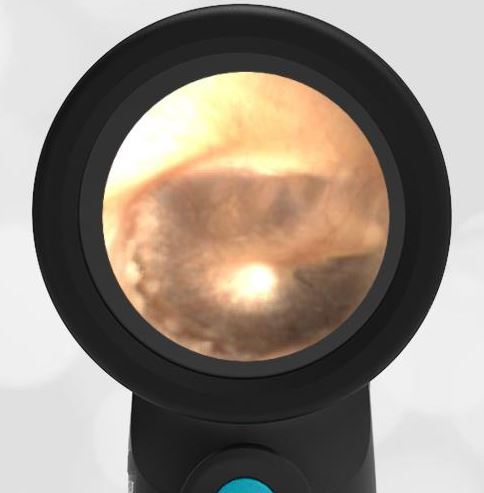
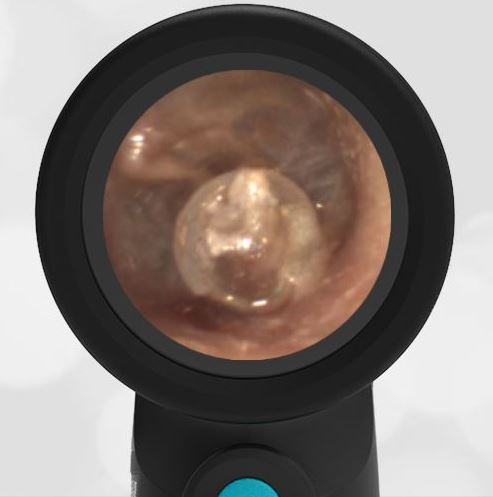
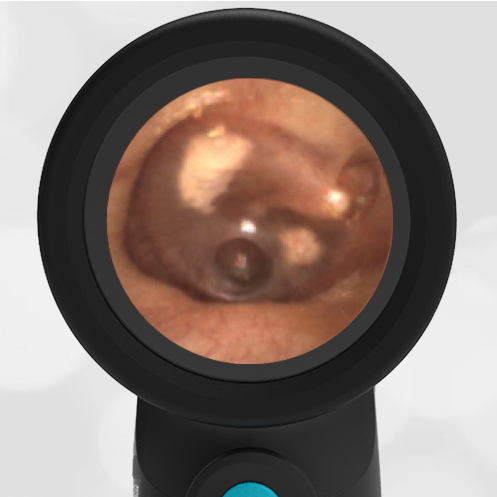
The child has hemotympanum (blood in the middle ear space).

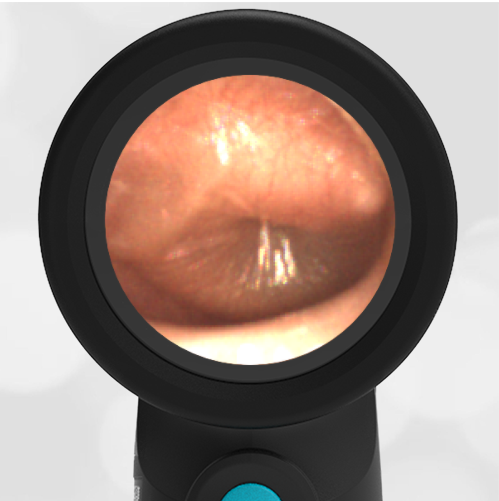
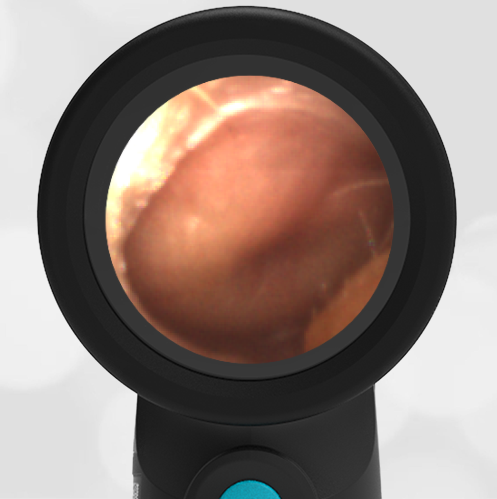
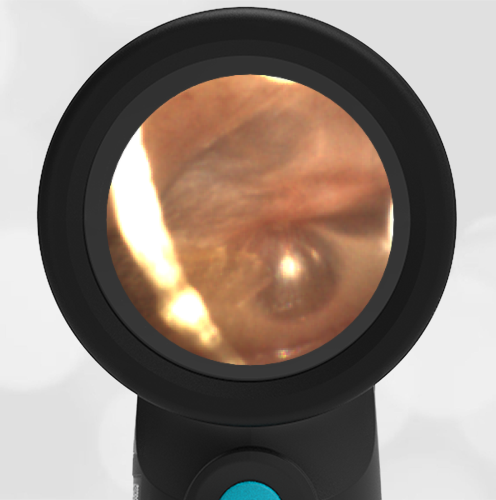
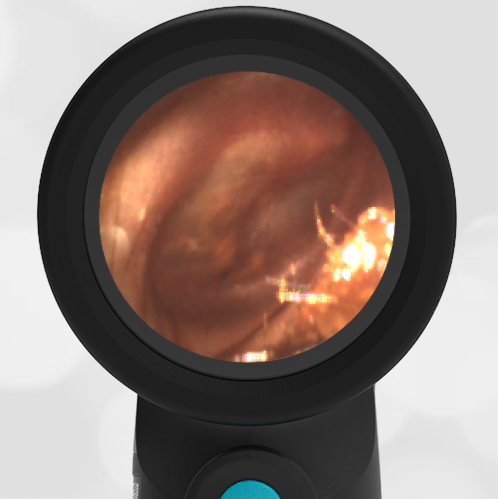
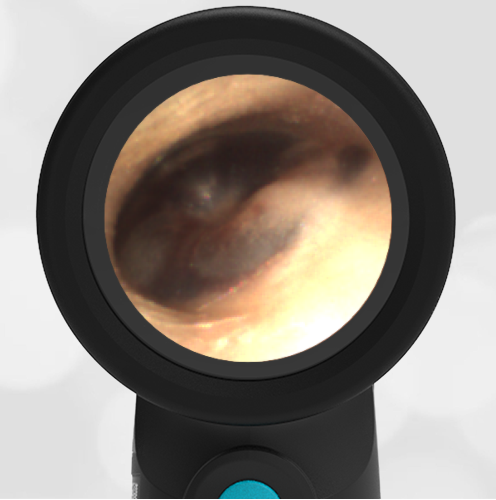
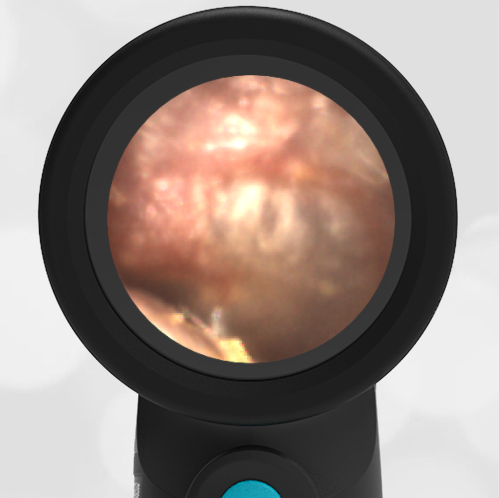
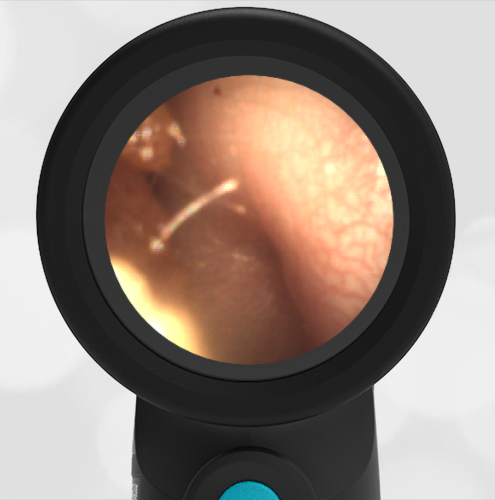
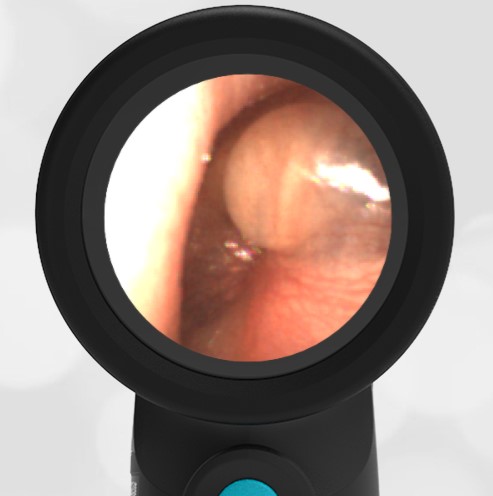
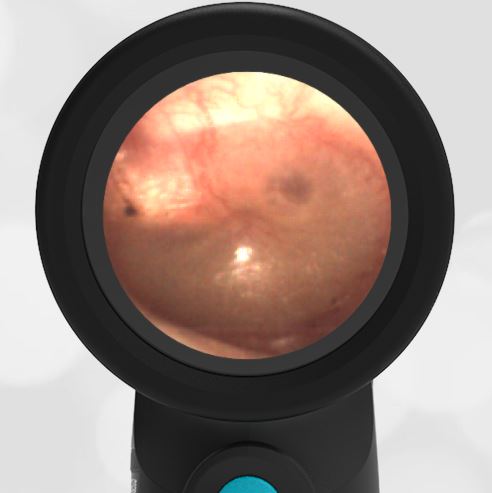
The child in this case has a right-sided hemotympanum as demonstrated by the dark-colored effusion and tympanic membrane hemorrhages noted in the anterior superior and inferior quadrants. With traditional otoscopy, this finding is easily missed since it requires a well-directed light onto the TM. Without this proper lighting, not to mention the cooperation from an injured child, a clinician is unlikely to confidently identify the hemotympanum. However, with the images captured via Wispr, it is quite easy to distinguish “a dark TM” from the normal uninjured side. Due to this previously missed finding of hemotympanum, a temporal bone CT was ordered that demonstrated a subtle fracture and effusion (blood) within the mastoid air cells. Fortunately, all of the child’s injuries were felt to be non-operative and he was able to be discharged with otolaryngology follow-up to ensure that the hemotympanum resolved without affecting his hearing.
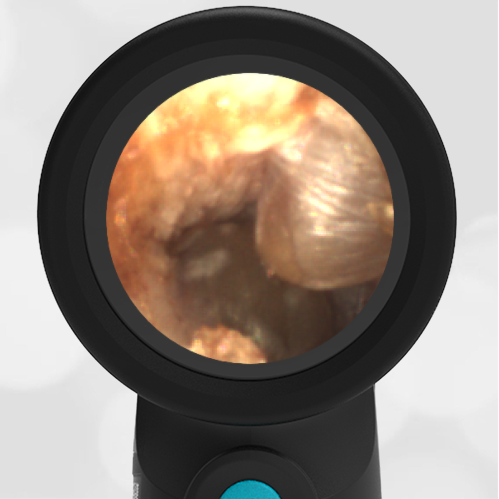
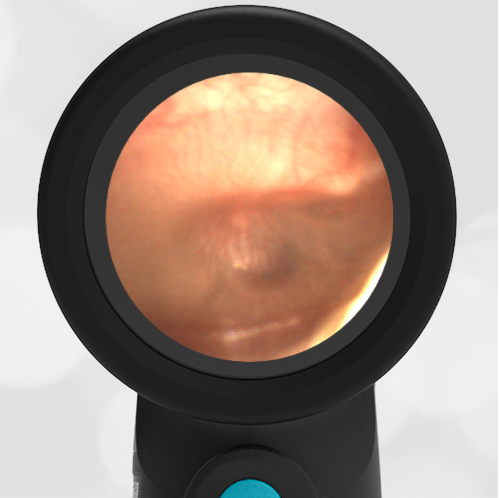
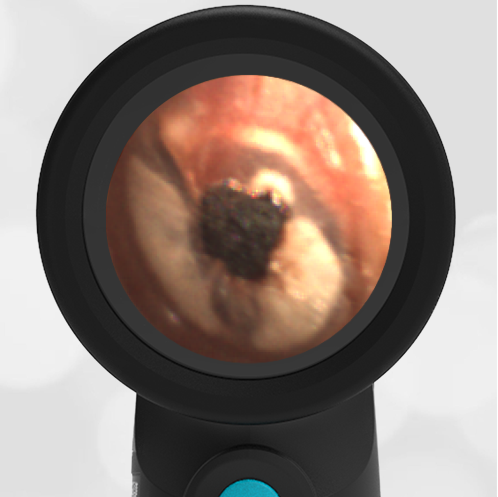
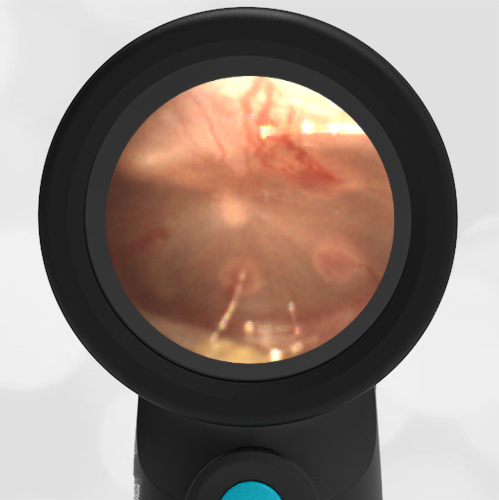
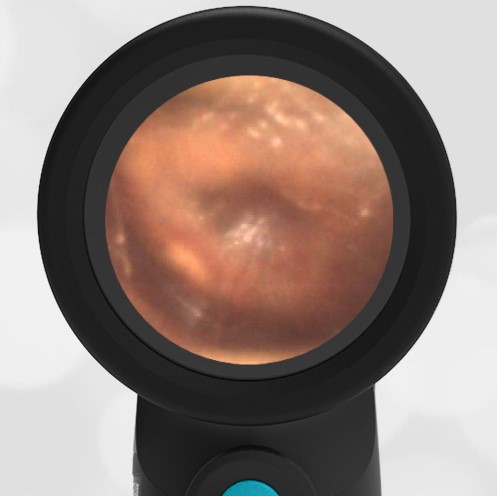
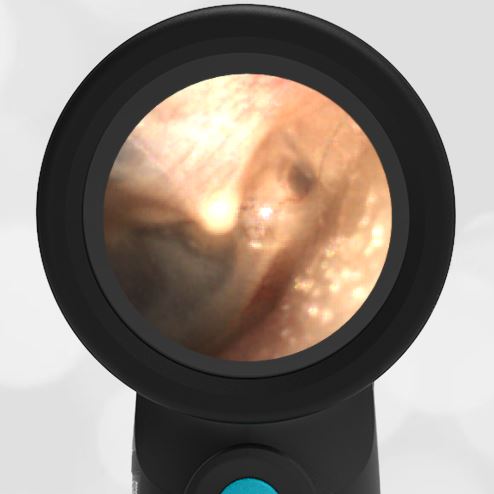
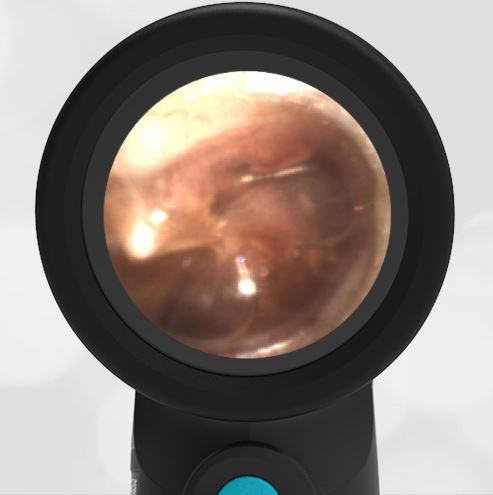
Here is another example of hemotympanum.